


Go to chapter: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | 29 | 30 | 31 | 32 | 33 | 34 | 35 | 36 | 37 | 38 | 39
Chapter 36 (page 181)




Go to chapter: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | 29 | 30 | 31 | 32 | 33 | 34 | 35 | 36 | 37 | 38 | 39
Chapter 36 (page 181)
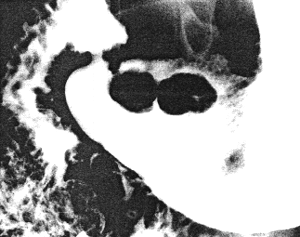 | Fig. 36.2 Case A.P. Peutz-Jeghers syndrome. A Sessile polyps close to pyloric aperture in relaxed pyloric sphincteric cylinder. |
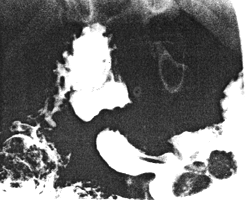 | Fig. 36.2 B.Sphincteric cylinder contracted. The polyps have moved in an orad direction |
A number of polyps were also seen in the second and third parts of the duodenum,
at the duodeno-jejunal junction and in the upper jejunum. A double-contrast barium
enema examination revealed no abnormality in the colon.
At endoscopy the presence of 2 sessile prepyloric mucosal polyps was confirmed.
In addition 2 smaller but similar polyps were seen in the body of the stomach; none of
the polyps had a stalk. Because of technical complications biopsies were not done. A
clinical and radiological diagnosis of Peutz-Jeghers syndrome was made. While under
investigation symptoms of upper small bowel obstruction supervened, necessitating a
laparotomy. A jejuno-jejunal intussusception was found and reduced. Gastrostomy,
duodenostomy and jejunostomy were done at which polyps were removed from the
stomach, duodenum and jejunum.
The histology of the gastric polyps showed prominent, branching processes of
muscularis mucosae with overlying columnar cell epithelium, without evidence of
dysplasia. The diagnosis of hamartomatous polyps of the Peutz-Jeghers type was made.
The patient made an uneventful recovery.
Previous Page | Table of Contents | Next Page
© Copyright PLiG 1998