



Go to chapter: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | 29 | 30 | 31 | 32 | 33 | 34 | 35 | 36 | 37 | 38 | 39
Chapter 13 (page 50)
Chapter 13
Radiographic Examination of Normal Motility
Introduction
In radiographic studies of the upper gastrointestinal tract, only the contrast material in the
lumen is visible, the actual walls of the tract being invisible.
The contrast material usually consists of one or more of the following:
- Insoluble, non-absorbable barium sulphate in fluid suspension. Where such a
suspension is used, it represents the luminal contents, and being radio-opaque, is
visualized as an image of positive contrast. In the "conventional" radiographic
study a low density barium suspension is used with a specific gravity of 2.004 and
a viscosity approximately four times that of water. The consistency approximates
that of thick soup but may, if required, be increased to that of a paste.
Commercial preparations contain additives regulating consistency and taste.
- Water soluble, absorbable iodine-containing solutions, also providing images of
positive contrast, but with lower radio-opacity than barium.
- Air, which may be swallowed or introduced via tubes, providing negative
contrast.
- Carbondioxide gas, affording an intraluminal, negative contrast agent. The gas is
liberated in the lumen by swallowed, commercially available gas-producing
granules or powders.
In the "conventional" radiographic study, barium sulphate with or without the addition of
air or gas is used, affording clear and sharply defined images of the contrast column in
the lumen. As pharmacologically active substances are not usually administered,
normally occurring, physiological movements of the contrast column may be studied.
While the rate of flow of a fluid contrast agent depends to a large extent on its viscosity,
we noted no naked eye differences in the type or range of movements, whether
"conventional" fluid barium suspension, barium paste or a watery iodine solution was
used as contrast agent. (Comment: The "range" of movement seen
radiologically roughly corresponds to the amplitude as determined at manometry).
The comparatively large volume of barium used in the conventional radiographic study
(much less being used in the double-contrast method) may obscure some of the
intraluminal features, confirming the dictum that "barium reveals but also conceals".
Consequently use is made of compression techniques, by which some of the suspension is
pressed away, to reveal the macroscopic mucosal folds and other intraluminal features.
In the double-contrast radiographic study, a coating of the luminal surface of the mucosa
is obtained by swallowing a small volume of a micropulverized, dense, more viscous
barium preparation; positioning the patient ensures equal allround coating. The
parenteral administration of an antimuscarinic pharmacological agent causes temporary
paralysis of the muscular walls with expansion of the lumen; this is enchanced by
introducing a large volume of carbondioxide gas into the lumen. Under these
circumstances naked-eye movements are no longer discernible; moreover, distension of
the lumen with stretching of the walls effaces the macroscopic mucosal folds. The
micropulverized barium enters minute furrows between the areae gastricae on the inner
surface of the mucosa, thus rendering the areae gastricae, or surface mucosal pattern,
visible (Fig. 13.1). In the present investigation, whenever motility patterns were studied,
the conventional barium examination was used.
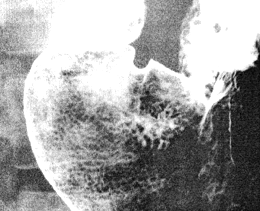 |
Fig. 13.1.
Double contrast study with gas distended lumen. Fine, reticular pattern
indicates areae gastricae or surface mucosal pattern
|
It is regarded as axiomatic in radiology that a temporary, circumferential, physiological
narrowing of the barium column in the lumen of a hollow muscular tube is due to
contraction of the walls of the tube. This supposition has not always been accepted
universally. It has been argued, especially in physiology, that a barium column may
appear to be narrowed in cases of incomplete filling of the lumen. Alternatively, even
with complete filling, a passive "falling together" of the walls (as opposed to active
contraction) may narrow the column. Whether these objections are valid or not may be
determined by combining alternative modes of investigation, e.g. manometry, with
radiological imaging procedures.
In the present context intraluminal pressure profiles and specially devised living
anatomical studies have been done in an effort to validate the radiological observations.
Previous Page | Table of Contents | Next Page
© Copyright PLiG 1998







