


Go to chapter: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | 29 | 30 | 31 | 32 | 33 | 34 | 35 | 36 | 37 | 38 | 39
Chapter 32 (page 157)




Go to chapter: 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | 29 | 30 | 31 | 32 | 33 | 34 | 35 | 36 | 37 | 38 | 39
Chapter 32 (page 157)
A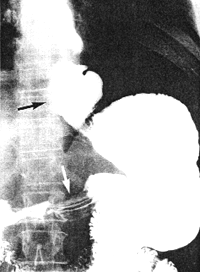 | 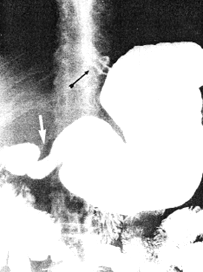 B B |
| Fig. 32.2 A,B. Case A.G.C. Large, sliding hiatus hernia (black arrows). Contracted pyloric sphincteric cylinder (white arrows) | |
It seems that, while the radiological abnormality may be unequivocal, the operative
findings, as far as the pyloric part is concerned, may be of an uncertain nature, as in the
following case:
Case 32.3. F.V., male aged 75 years, was admitted for mild obstructive jaundice of 10
days' duration. There had been colicky epigastric pain for the previous 5 months, as well
as acidity and heartburn for years. Oral and intravenous cholecystography revealed poor
concentration of the opaque medium with calculi in the gallbladder and a dilated common
bile duct containing stones. (At the time sonography of the gall bladder had not been
perfected). The radiological examination showed a large, irreducible hiatus hernia (Fig.
32.3). A contraction of the pyloric sphincteric cylinder, 4.5 cm in length, with a tendency
toward formation of a pseudodiverticulum on its greater curvature side, was constantly
present; there was no evidence of any other lesion locally or in the remainder of the
stomach. The diagnosis of contracted pyloric sphincteric cylinder, resembling AHPS, in
association with hiatus hernia was made. At operation a cholecystectomy was done and
calculi were removed from the common bile duct. The surgeon stated that the pyloric
area of the exposed stomach felt a little thicker than usual. Had his attention not been
drawn to it beforehand, it is doubtful if he would have commented on it in his operative
notes. No other gastric lesion was detected. Because of the patient's age, it was decided
not to repair the hernia at that time. Repeat radiographic examination 5 months later
showed the irreducible hiatus hernia and the contracted pyloric sphincteric cylinder to be
unchanged.
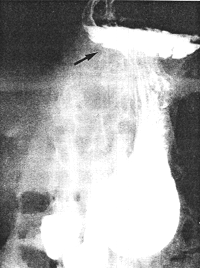 |
Fig. 32.3. Case F.V. Large irreducible hiatus hernia (black arrow). Contracted pyloric sphincteric cylinder |
In this case two points are worth noting:
Previous Page | Table of Contents | Next Page
© Copyright PLiG 1998